Mathematica has released findings from their evaluation of the first year of the Primary Care First model. The study found that most practices entered the model with advanced primary care capabilities already in place, especially in the areas of access and continuity, care management, and patient and caregiver engagement. The majority of changes made in the first year were largely enhancements of existing activities and hiring additional staff. The findings-at-a-glance document and full report summarize the research.
Through the Primary Care First model, the Centers for Medicare & Medicaid Services (CMS) Innovation Center is testing whether an alternative payment model will increase patients’ access to enhanced primary care services, which should, in turn, improve quality, improve patient experience of care, and reduce expenditures for Medicare beneficiaries. This model uses a payment model that requires practices serving fee-for-service Medicare beneficiaries to take on upside and downside financial risk. Practices receive a flat visit fee and a prospective population-based payment that varies by the health of their patients. Payments will be adjusted based on performance starting in the second year.
“The Primary Care First model is an important step towards shifting traditional Medicare reimbursement to value-based payments in the primary care setting as well as supporting CMS’s goal in ensuring that a greater proportion of patients are receiving care through an accountable care arrangement,” said Leslie Conwell, lead author and principal researcher at Mathematica. “Our findings suggest that practices embraced the opportunity to implement strategies that will lower hospitalizations and expenditures while improving care for their patients.”
Primary Care First is an evolution of several other advanced primary care models tested by CMS that aim to improve care and lower costs. Mathematica evaluated these models, which include the Comprehensive Primary Care model and the Comprehensive Primary Care Plus model. Insights from these evaluations have provided decision makers important evidence about what works to continue strengthening primary care and its vital role in keeping people healthy.
This is one of the largest advanced primary care models tested by CMS. There were 846 practices across 26 regions that joined the first cohort in 2021. These practices include more than 4,000 practitioners that serve over 500,000 Medicare beneficiaries. A second, much larger cohort of over 2,200 practices joined in 2022. In 2021, practices were supported by CMS and 13 public and private payers.
Number of practices in PCF Cohorts 1 and 2 in 2022, by county
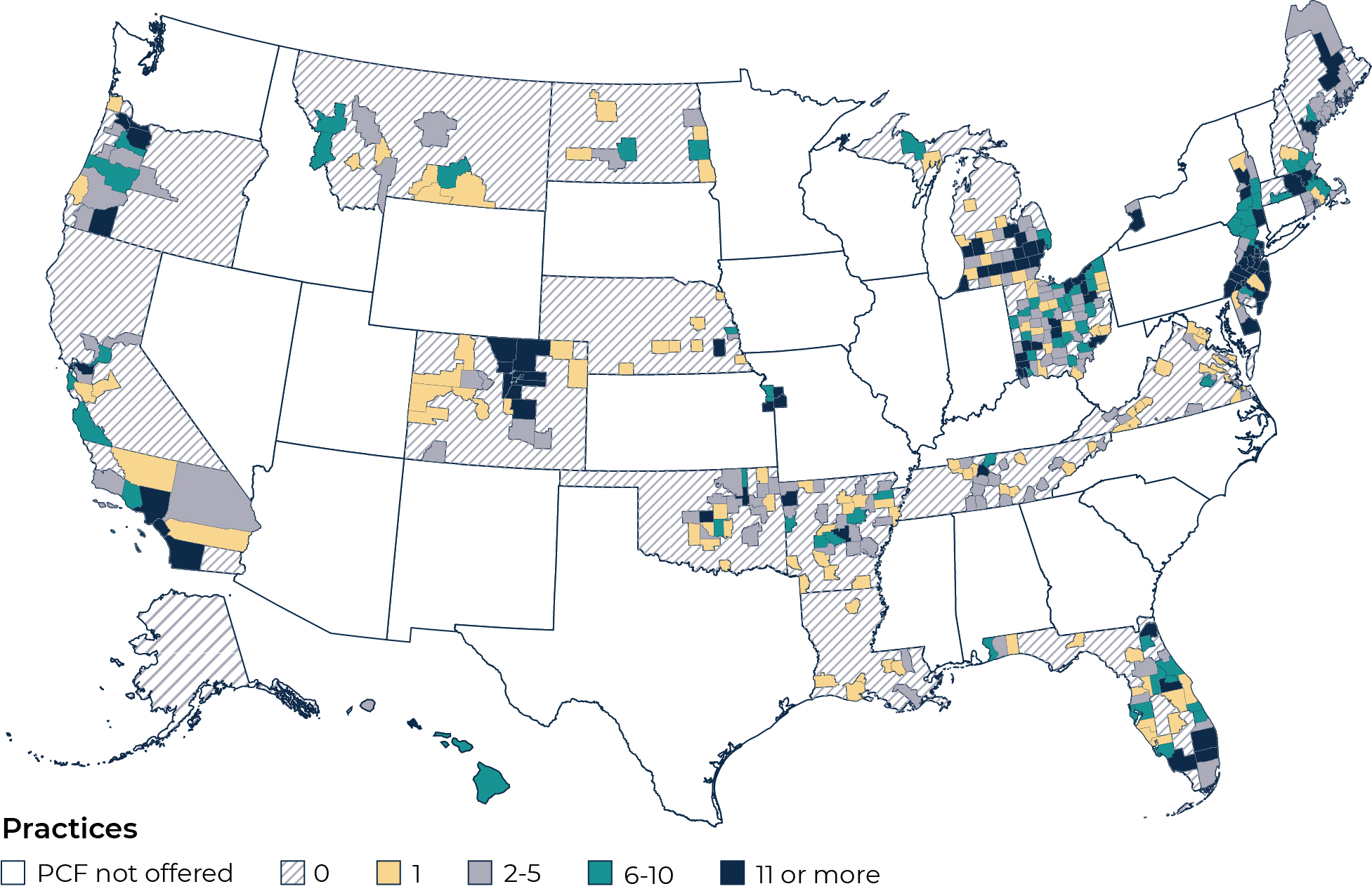
Stay tuned for more results from the evaluation. Future reports will describe how practice activities result in improvements in quality of care and lower acute hospitalizations and total cost of care for Medicare beneficiaries and will explore how the model may affect health equity.
Contact
-
Christal Stone Valenzano
cstone@mathematica-mpr.com
202-420-0691


